The 18th annual “Create the Future” Design Contest for engineers, students, and entrepreneurs worldwide, sponsored by COMSOL, Inc., and Mouser Electronics, drew more than 750 innovative product ideas from engineers and students in 60 countries. Analog Devices and Intel were supporting sponsors, and Zeus sponsored the medical category.
For the first time ever, readers are invited to join us November 10 for a special one-hour presentation as we honor our 2020 Grand Prize Winner, along with the winners in seven categories. Visit here for more information and to register to attend.
This preview introduces the finalists in the Medical Products category. The medical winner and honorable mentions will be featured in the December issue of Medical Design Briefs. Entries for all categories can be viewed here .
Wound Healing Patch

This novel wound healing patch is designed for use with adhesives or bandages at the wound site. The engineered patches resemble the natural tissue structure found in the body. The structures act as supports for the cells, guide cell growth and alignment, and help in accelerating wound healing, thus reducing scarring and preventing secondary infections. The one-time use patches are optimized for different wound types using polymer materials that are biodegradable, biocompatible, and FDA approved.
In addition to being constructed for specific wound types, they can be customized by size, and they can include drug release over time or antibacterial protection. Once administered, the patches promote cell growth, provide structural support to new tissues, and strengthen the wound bed, thus providing protection from repeated trauma. The patches could significantly reduce healing time in chronic wounds such as diabetic foot ulcers from a year to a few months and improve a patient’s overall quality of life.
For more information, visit here .
Wearable Continuous Blood Pressure Monitor

A comfortable and easy-to-use wearable device has been developed for continuous blood pressure (BP) monitoring and management over long periods of time. The device provides timely data to treat patients at risk of rapid changes in blood pressure that can lead to stroke or multiple organ failure, while removing the pain and risk of the current standards of care at a lower cost and increased patient compliance.
The device uses paper-thin capacitive sensors lightly contacting the skin. The sensors pick up a pulse waveform signal that correlates to arterial blood pressure changes. Artificial intelligence models extract BP values that meet the FDA’s accuracy guidelines for noninvasive blood pressure monitoring.
For more information, visit here .
Implantable Wireless Pacing System

Eliminating the need for wires and batteries in ICDs and pacemakers is highly significant. Traditional ICDs and pacemakers send electrical pulses to the heart through wires called leads. Leads, however, cannot always be placed where needed, and they are prone to infection and fracture.
This miniaturized implantable wireless, battery-less pacing system (nodes) consists of tiny silicon-based integrated microchips. Each node weighs only about 0.09 g because it requires no internal batteries. Because it can deliver pacing not only to any location but to an unlimited number of locations on the heart, this technology has the potential to deliver imperceptible (painless) defibrillation through sophisticated, coordinated, and targeted multisite pacing bursts.
For more information, visit here .
Wearable Blood Glucose Monitor
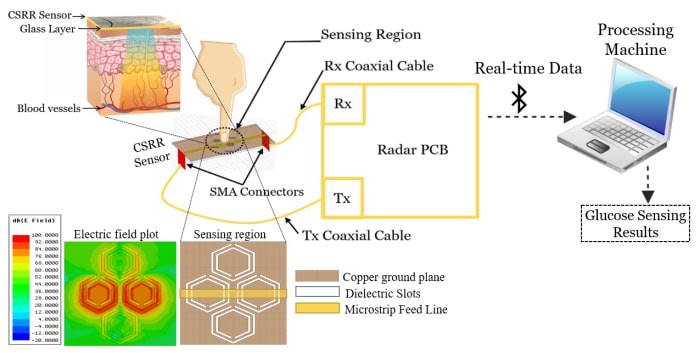
A compact low-cost wearable sensing system utilizes microwave sensors and artificial intelligence to enable diabetics to noninvasively monitor their blood glucose levels without sampling any fluid outside of the body. The device sends electromagnetic signals of small wavelengths through the finger skin. Signatures of blood glucose levels are reflected in the sensor-scattering responses that are further analyzed to identify the blood glucose levels accurately.
The sensor design incorporates four cells of complementary split ring resonators (CSRRs), arranged in a honey-cell configuration and fabricated on a thin sheet of a dielectric substrate. The CSRR elements are coupled via a planar microstrip-line to a radar board operating in the ISM band 2.4–2.5 GHz. The enhanced design of the CSRR elements intensifies the electric field over the sensing area in the near-field region, thus allowing the sensor to detect small variations in the electromagnetic properties that characterize the varying glucose levels. Therefore, placing the fingertip over the sensing region would consequently perturb the distribution of the highly concentrated electric field.
For more information, visit here .
Blood Test for Early Lung Cancer Screening

A revolutionary technology enables earlier lung cancer screening to diagnose the disease when it is more treatable. The eXoutcancer system combines a nanochip and a proprietary spectroscopic database derived from a machine learning (ML) algorithm. The biomarker that the device is detecting is called an exosome. Cancer cells release a larger quantity of exosomes, which are found throughout various cancer stages. Because the exosome is a routine cellular process, it’s found throughout each cancer stage.
A key advantage of the system is the combination of a nanochip and a technique called surface-enhanced Raman spectroscopy (SERS). When a laser is scanned across the chip’s surface, any exosome near the nanofeatures gets its signal enhanced, giving the platform the ability to measure at the single exosome level. This translates to extremely high sensitivity and specificity, even at low concentrations. The complex spectroscopic data is parsed out via an ML algorithm to develop this diagnostic fingerprint.
For more information, visit here .




