While pacemakers have been instrumental in treating many patients with heart rhythm disorders, their bulky design and dependence on wires can limit their usefulness and poses a risk of heart damage or infection. Researchers have cut the cords, shrunk the size, and expanded the capabilities of current designs.
Their new technology is a lightweight, flexible silicon membrane that conforms to the surface of the heart, delivering electrical current when and where beams of light strike the device. The researchers used their strategy to regulate heart activity in a variety of live animals. The results suggest the system could someday provide a high degree of control over irregular heart activity while placing less risk and burden on patients than traditional pacemakers.
The method enables more freedom to adjust the stimulation location. This freedom stems from a process called the photovoltaic effect, wherein light rays cause a material to produce an electric current. The new pacemaker technology mirrors the structure of a solar cell — its two silicon layers primed to facilitate electrical flow — but instead of storing the electrical charge, the device distributes it onto the underlying heart muscle below.
The pacemaker device was first evaluated in samples of cardiac cells and ex vivo animal hearts. By shining a laser on the membrane, they successfully triggered contractions in both models. Next, they tested their method in live mice, rats, and pigs. After applying the device, the team stimulated heart tissue at various locations, sometimes simultaneously. This coordinated stimulation is critical for a heart failure treatment called cardiac resynchronization therapy (CRT). With CRT, physicians utilize pacemakers to restore and coordinate activity across the heart’s upper and lower chambers.
Throughout all experiments, the resarchers succeeded in stimulating hearts to beat steadily across a wide range of target rates using healthy animals. In one experiment they obtained similar results in an injured heart model. The outcome of these tests was promising but limited by the fact that they used a highly invasive approach to place the device on the heart and stimulate it with a light source.
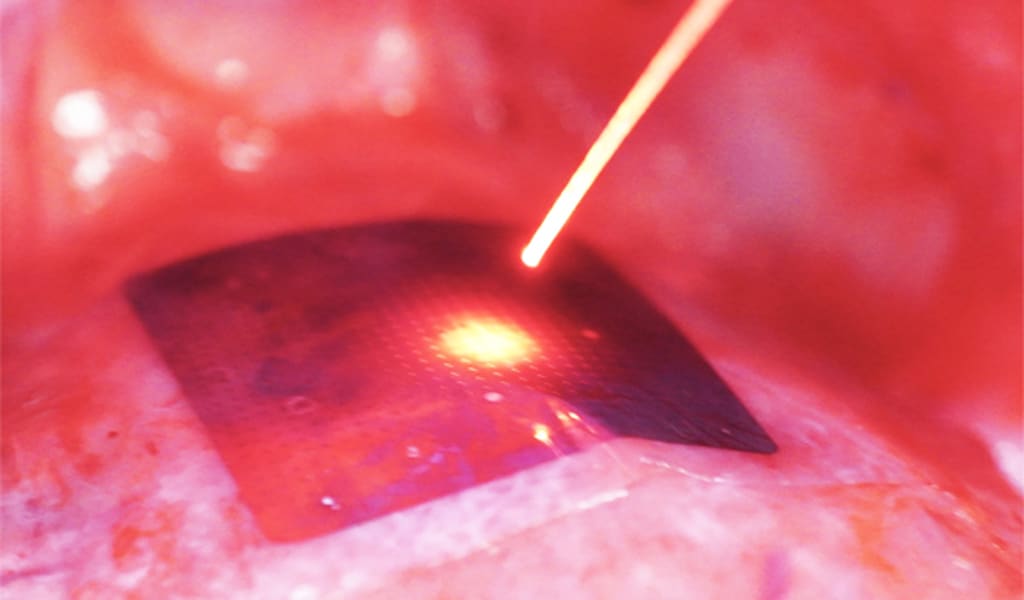
The team devised a less-intrusive procedure for their final test, conducted in a live pig. They inserted a collapsed version of their device through a small incision to position it on the heart. Then, the researchers slid an optic fiber through the same opening to shine light on the device and regulate the animal’s heart rate.
While the study proved that the new approach holds water for short-term procedures such as CRT, the researchers believe that their device could find use in long-term applications. For treatment of chronic conditions, a small, wireless LED implanted under the skin of a patient could remotely trigger stimulation.



