Today's imaging systems save lives by making the unseen visible to a degree never before possible. Medical professionals can now view systems within the human body in high resolution, enabling them to diagnose pathological changes while precisely targeting therapeutic procedures. From the operating room to telemedicine, these imaging technologies play a key role in the future of medical diagnostics and therapeutics.
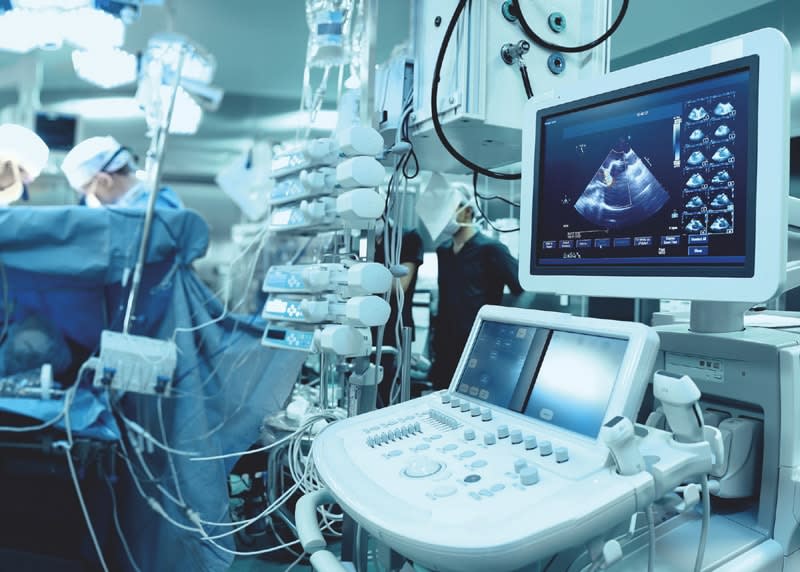
However, medical professionals face challenges connecting the images to healthcare processes more quickly and more accurately for better patient care and outcomes. Leaders in the medical imaging space require new technology providing higher resolution images and faster image reconstruction, while also enabling an improved user interface that incorporates multiple images and patient vitals. Digital transformation initiatives require that these complex devices transfer images and data throughout the entire healthcare ecosystem securely, reliably, and in real time. In order to meet the needs of this rapidly changing industry, the adoption of commercially available, data-centric communication technology is paramount to control costs and shorten time to market.
What's Driving Innovation?
A number of forces are shaping the future of medical imaging: an increase in CPU performance; the availability of certifiable, off-the-shelf software; the increase in adoption of minimally invasive, image-guided surgery; and the desire to connect all healthcare and medical devices to leverage the data generated throughout the ecosystem.1
Advances in CPU performance, mainly due to the addition of graphics processing units (GPUs) over the past decade, have been nothing short of amazing. Since 2008, CPU performance has increased roughly 100x, increasing demands on other technology components within a system. Today's high-performance CPUs enable data transfer of >25 GB/sec, the equivalent of streaming 2000 HD videos, requiring an internal communication protocol that can meet that level of performance. The 3D images produced by CT, ultrasound, MRI, and PET scans are computationally intensive. GPUs allow parallel processing to break down complex computing problems into many smaller tasks that run simultaneously, speeding up diagnostics, lowering patient radiation and improving image reconstruction time by over 100x versus legacy quad core CPU based designs.
While computing hardware has become orders of magnitude faster, software development to leverage this power can still be painfully slow. The most innovative imaging companies are increasing their use of commercial off-the-shelf software, taking advantage of this new hardware while decreasing time to market. Until recently, it was common for medical imaging R&D teams to design, build, and maintain the vast majority of the software within their systems. Much of this software was not a core competency but rather an enabling technology like a real-time operating system (RTOS), a communication protocol, or even a UI/UX. There are now a number of options in each of these spaces that not only meet the technical requirements of the medical imaging market, but also provide a certifiable, medical-grade offering. The most successful imaging companies make use of these commercial offerings, increasing the performance, security, and reliability of their systems while freeing up their development teams to focus on their core skills related to building and interpreting medical images.
Image-guided minimally invasive surgery (MIS) is growing at a rapid pace, driven by the constant flow of positive outcomes. Surgeons now perform procedures using a combination of real-time and archived images of a patient. Image-guided surgery provides surgeons with greater control of the surgical procedure, real-time feedback on the effect of the intervention, and reduced tissue trauma and disruption in gaining access to the anatomical structure.
Procedures using CT, MRI, and PET were developed for the treatment of brain tumors, but now the practice has been expanded to include additional imaging techniques and to treat additional modalities. High-definition 3D images and the ability to overlay different image types opens the door for a number of new image-guided minimally invasive surgical procedures that can be performed with extreme precision. Improving patient outcomes and lowering the cost of care will drive continued growth of advanced imaging in concert with MIS.
The last trend shaping the medical imaging industry is the most significant and disruptive of our lifetime. We are moving from a world and a healthcare system that is generally unconnected to one that is always connected, transmitting huge amounts of data securely, reliably, and in real time. Data will be shared not only within each medical imaging subsystem, but within a larger system of care. Non-interoperable systems where data today is siloed and unreachable will be replaced by interoperable healthcare IoT systems able to share data, analyze, diagnose, and eventually provide treatment based on artificial intelligence (AI) and machine learning (ML).2 The requirements of this type of system mirror those of a stand-alone medical imaging system; however, now requirements for performance, reliability, and security must scale throughout the larger healthcare Industrial Internet of Things (IIoT) system. The healthcare IIoT is coming, and medical imaging architects need to be considering how they integrate into these larger systems.
The Challenges
Architecting and developing a medical imaging device isn't easy; development cycles range from four to six years. Even by adopting the latest technologies, device designers still run into challenges striving to meet next-generation product requirements, many of which are related to connectivity. The most significant technical challenges are outlined below:
Performance. Systems will need to transfer 4k ultra HD images/video (>40GB/s) with >10 ms latency.
Reliability. Catastrophic failure in an image-guided minimally invasive surgery is not an option.
Interoperability. The ability to seamlessly communicate with complementary medical devices, additional imaging equipment, and the larger healthcare IIoT.
Security. The need to meet strict regulatory compliance while adding connectivity to a wide ecosystem of devices increase the potential for data exposure and vulnerabilities.
Scalability. The need to architect a communication framework that not only meets the requirements of the next-generation product, but also scales within the healthcare IIoT.
Not all challenges are technical; some of the most significant challenges for medical imaging come from the business side. Maintaining product design cycle times, staying within budget, and minimizing long-term cost of ownership are challenges facing medical imaging executives as their teams address next-generation market needs.
The Solution
The solution is to use commercial off-the-shelf (COTS) data-centric connectivity framework to handle software integration within the imaging devices and to share data with other systems in a wider healthcare IoT. What is data centricity? Data-centricity is an architecture in which the interface between systems or subsystems is the data itself. There are no artificial wrappers or blockers to the interface (i.e., no messages).
In data-centric systems, the underlying infrastructure understands that data, which decouples applications from the data, removing much of the complexity in application development. Data-centric systems manage the data and provide rules on how the applications exchange data, providing a single source of truth.
An example of a data-centric technology that is addressing the design challenges of the next generation medical imaging systems is the Data Distribution Service (DDS) standard. DDS is an open, multi-vendor, data-centric connectivity standard. DDS has roots in mission-critical, high-performance defense, industrial, and embedded applications.
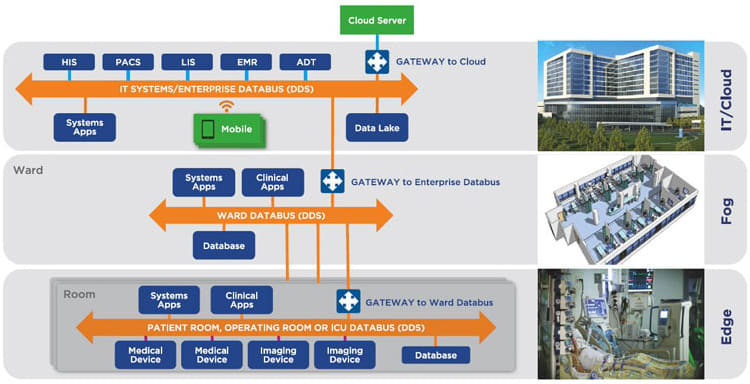
DDS introduces the idea of a databus, a shared global data space that can efficiently deliver millions of messages per second to many simultaneous receivers, while offering detailed quality of service (QoS) control, multicast, configurable reliability, and pervasive redundancy. It is the only technology that delivers the flexibility, reliability, and speed necessary to build complex, real-time applications, a perfect fit for medical imaging (see Figure 1).
A data-centric DDS-based architecture (see Figures 2 and 3) can address the challenges of connected medical imaging, as follows:
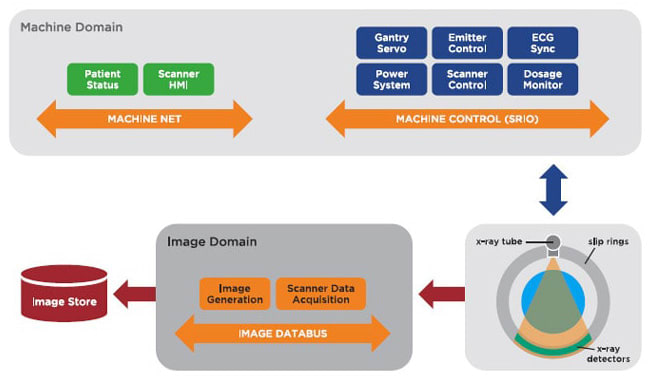
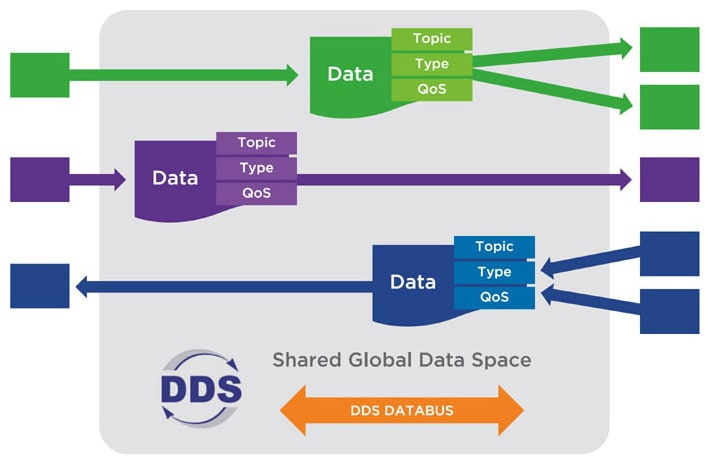
Performance. DDS was constructed from the ground up for real-time control of cyber physical systems over a network. Specific features like zero copy/shared memory, QoS, flat data, and data filtering allow DDS to meet the latency and throughput requirements specified of the most demanding imaging applications.
Reliability. DDS enables the use of redundant paths and by design does not have a single point of failure.
Interoperability. DDS provides syntactic interoperability allowing for a common communication protocol providing a foundation for healthcare IIoT integration.
Security. DDS is a key piece of a trusted security architecture by providing fine-grained security down to the level of the data, not just the “pipe.”
Scalability. DDS-based systems provide near-linear scalability, automatic discovery that provides plug-and-play functionality, and enables bridging to other technologies via routing service.
The medical imaging market is experiencing a period of rapid innovation driven by new technology and cutting-edge customer requirements. To enable innovations in both interventional and diagnostic radiology, it is clear that these systems and their subsequent subsystems will need to be interoperable and move more data, in real time, reliably and securely.3
Utilizing a data-centric system architecture based on standard connectivity technology like DDS allows R&D teams to meet strict design requirements without building their own proprietary connectivity solution from scratch. Commercial DDS offerings like Connext DDS from RTI, for example, offer the most significant benefit by providing a medical-grade DDS that allows medical imaging manufacturers to focus on implementing next-generation product features and leaving the connectivity to the experts. This approach has proven to save development time and speed time to market by allowing all parties to focus on their particular area of expertise: saving lives and improving patient outcomes.
This article was written by David Niewolny, Director, Healthcare Market, Real-Time Innovations, Inc. (RTI), Sunnyvale, CA. For more information, visit here .



