Steven Conrad, MD, PhD, an emergency and critical care physician at Louisiana State University Health Science Center, New Orleans, is not your typical physician. When he’s not conducting rounds on patients or teaching residents in internal medicine, emergency medicine, or pediatrics, this biomedical engineer is using multiphysics simulation to optimize the design of artificial kidneys. Using COMSOL Multiphysics, Dr. Conrad simulates the hollow fibers that make up a dialyzer, using computer aided engineering (CAE) tools to advance the design of artificial kidneys. The simulations that he creates don’t just optimize current dialyzer designs—his simulations improve upon them by taking into account physical properties that weren’t considered in previous designs, and even allow for dialyzer improvements and optimizations on a patient by patient basis. By improving the functionality of artificial kidneys, he hopes to create artificial kidneys that will revolutionize the dialysis process.
Multiphysics Simulation Transforms Biomedical Practices
Until recently, artificial organs were frequently designed empirically, with little or no simulation involved in the design process. As multiphysics simulation software emerged as a valuable analysis tool for scientists and engineers, its capacity for improving biomedical designs became apparent as well. The versatility and flexibility of the multiphysics approach allowed doctors to simulate biological processes and incorporate more physics into a design than was previously possible. In the past decade, multiphysics simulation has been used to study heat transport in organs, fluid-structure interaction in the brain, and musculoskeletal structural analysis, among others. Multiphysics not only allows more than one physics in the simulation process, but also takes into account resulting interactions that occur between coupled physics effects.
As multiphysics simulation was used to improve on various applications in medicine and biology, Dr. Conrad decided that they could prove vital to designing accurate and efficient dialyzers as well. Using COMSOL Multiphysics, he simulated, analyzed, and optimized artificial kidney designs. “I felt that by using simulation in the design process, I could create artificial kidneys with higher efficiencies than the ones that were currently being used,” he stated.
Renal Replacement Therapies
One in nine American adults currently suffer from chronic kidney disease (CKD). Nearly half a million of those patients have progressed from CKD into end-stage renal disease (ESRD), and currently require dialysis or transplant therapies just to stay alive. With the number of patients entering ESRD increasing by 5 to 10 percent per year, providing efficient and cost-effective dialysis treatments is a growing issue in the medical field.
A healthy kidney filters fluids at a rate of 90 mL per minute or more, a process that is measured by the glomerular filtration rate (GFR). A patient with renal failure has a decreased filtration rate described in stages, with Stage 5 (GFR of <15) defined as ESRD, and requires dialysis. When a patient is diagnosed with ESRD, they begin dialysis treatments three to five times per week. However, recent studies have found that even these treatments, which last anywhere from three to five hours per treatment, may not be doing enough. By optimizing and improving the effectiveness of dialysis treatments, doctors may be able to not only improve upon a patient’s quality of life, but their life expectancies when on dialysis as well.
Renal replacement therapies, such as dialysis, involve the removal of electrolytes, excess water, and metabolites that build up in the body due to kidney failure. There are a few different types of renal replacement therapies, but three of the most common are hemodialysis, hemofiltration, and peritoneal dialysis.
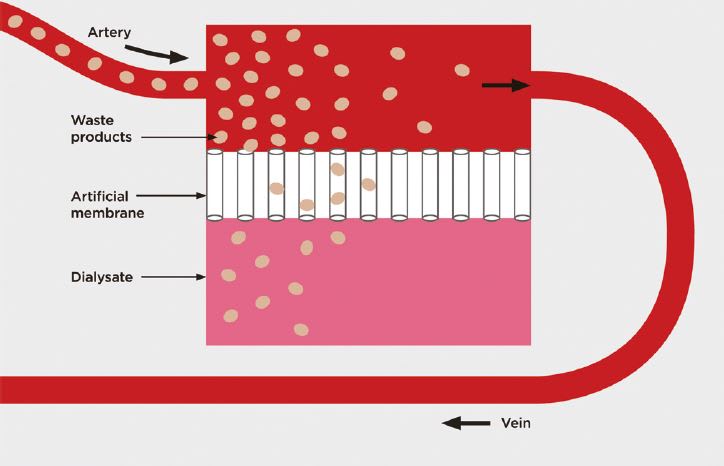
Hemodialysis and hemofiltration are the most common, and use an external dialyzer to filter blood, usually removed from an arteriovenous fistula in the patient’s arm. Hemodialysis is the more traditional form of dialysis, relying on diffusive transport and low porosity membranes to remove small, toxic, and easily diffusible solutes from the blood, such as creatinine and urea. (See Figure 1)
Hemofiltration relies on convective transport to clear solutes, and is able to remove larger or mid-sized solutes, now known to contribute to toxicity, in addition to smaller solutes. Using hydrostatic pressure, hemofiltration drives both small and large molecules through a filtration compartment where molecules are removed by a porous membrane made up of hollow fibers.
Currently, therapies involving a combination of both hemofiltration and hemodialysis, called hemodiafiltration, are common and result in a more complete removal of both small and large toxins.
How to Improve Hemodiafilter Design
A hemodiafilter is a dialyzer used in the hemodiafiltration process. The dialyzer is composed of axisymmetric hollow fibers that make up an artificial membrane and a fluid called the dialysate that catches and separates the toxins and solutes from the blood. Using COMSOL Multiphysics, Dr. Conrad simulates the interaction between hollow fibers, blood, and dialysate fluid, which are non-Newtonian fluids. By creating an accurate model of the hemodiafilter, and incorporating all important physical effects into one simulation, he is able to create designs that more accurately predict fluid flow and solute transport during the dialysis process.
Previous simulations of fluid flow in artificial kidneys used simplified lumped-compartment models that failed to account for the complex interactions that govern blood flow and species transport. These models oversimplified the blood filtration process and, therefore, failed to fully predict the behavior of membranes, such as the effect of pressure distribution and the interactions of molecules of varying size within the dialyzer. Dr. Conrad’s simulations incorporate these factors, and allow for a more accurate picture of the interactions taking place inside a dialyzer than was previously possible. Using COMSOL, he is able to include all of the physics that are known to affect fluid flow and solute transport in one simulation. Processes that were previously simplified or left out of the equation entirely are now included to create a simulation that demonstrates improved accuracy when compared to experimental data.
All-Inclusive Dialyzer Simulation

One of the key areas of improvement in Dr. Conrad’s research is his simulation of the porous membranes that line the hollow fibers. Previous simulations considered the membranes of these hollow fibers without taking into account near-membrane interactions—an approach that was unable to account for the interactions that occur between blood and membrane. These interactions include the Fahraeus-Lindqvist effect on hematocrit, solute backfiltration, hydraulic and osmotic pressure gradients, solute and protein concentration gradients, non-constant concentration polarization along the membrane border, and convection and diffusion principles. By simulating these interactions at the membrane itself, Dr. Conrad is able to more accurately predict both the convective and diffusive transport that takes place across the membrane.
Not only does convection and diffusion across the porous membrane affect dialysis, but complex interactions affect the process as well. One complication is backfiltration, which takes place from the dialysate back into the filtered blood. This solute flux is the result of hydraulic and osmotic pressures that build up between the membranes of the dialyzer and drive forward and back filtrations. Dr. Conrad’s simulation used the Navier-Stokes and Brinkman equations to predict backfiltration under such conditions, and take into account the increasing solute concentrations and pressures of the dialysate as the blood continues down the dialyzer. To further complicate the process, the dialysate has a cooler temperature than blood, and heat loss to the environment must also be taken into account, which can be coupled and simulated with the multiphysics approach.
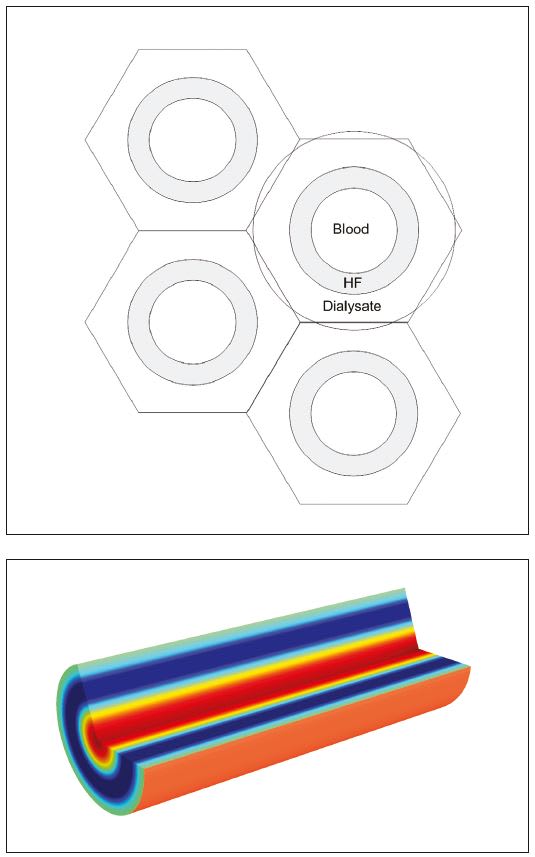
Another specific way in which Dr. Conrad’s dialyzer improves on previous simulations is the way in which pressure gradients and solute concentrations are described along the length of the dialyzer fibers. For example, as the filtration processes continues along the length of the hollow fiber, there is a drop in pressure that occurs as solutes continue to be filtered out of the blood and into the dialysate. Previous models would predict fluid flow along the fiber using a length-averaged mass transfer coefficient, instead of an adaptive formula using partial differential equations (PDEs). By using PDEs and incorporating equations associated with the Fahreaus- Lindqvist effect, which explains how blood viscosity decreases as the hollow fiber apparent diameter decreases, these new simulations can account for the changing conditions that occur along the entirety of the hollow fiber and, therefore, more accurately predict particle and solute behavior across the fiber membranes. (See Figures 2a and b)
In addition to examining transport processes in the hollow fibers, Dr. Conrad is also looking at blood flow in the grafts used for vascular access, which have an unacceptable failure rate. An example of the complexity of these simulations can be seen in Figure 3. Secondary flows in the ligated arterial segment and swirl flows in the graft segment are easily identified. Simulation can predict the pressure loss in the circuit, and provide insight into the deterioration of the graft function over time. “Vascular access complications represent the greatest cause for hemodialysis patient hospitalizations,” said Dr. Conrad. Simulation can help understand and prevent these complications and optimize fluid flow from vascular access grafts.
The Future of Dialyzer Designs: Optimization One Patient at a Time
With these improvements in dialyzer designs, Dr. Conrad hopes to advance the dialysis process. His approach will eventually allow for dialyzer optimization through adjustment of operating parameters and the improved configuration and design of membranes. By optimizing the length, number, and materials used to construct the hollow fibers, the entire process can be improved. By using more accurate simulations, his designs can account for continually changing spatial variations of physical parameters like viscosity, diffusion, and kinetic coefficients. Future studies will extend his simulation to include membrane polarization and particle charge, allowing for a more complete simulation of all physics effects involved.
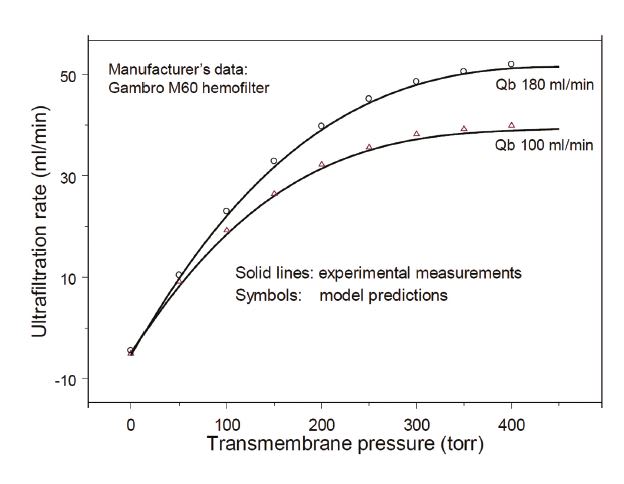
While experimental testing is not complete, so far, his simulations have demonstrated excellent agreement between measured and simulated data. (See Figure 4)
By verifying and optimizing dialyzer designs, the future of renal replacement therapies could be revolutionized. Because Dr. Conrad’s simulations afford a more complete picture of the interactions taking place within the hemodialyzer, they allow for the possibility of dialyzers to be modified and manufactured to account for varying patient and operational parameters.
This article was written by Alexandra Foley, Technical Writer, COMSOL, Inc., Burlington, MA. For more information, Click Here



